 On the other hand, although your patients may not appreciate how sick they really are, they will certainly remember any pain you inflict. Sedation: Sure, a little pain is better than death.Positioning: An anterior-posterior pad positioning is probably better than anterior-lateral.Dose: Use full dose electricity on the first attempt (200 joules on my biphasic machine).However, I will generally give cardioversion an initial shot. Unfortunately, cardioversion never seems to work in these really sick patients. The patient is unstable, so electrically cardiovert him. CardiovertĪccording to the ACLS guidelines, management is very straight-forward. If in doubt, make sure to search for alternate causes of shock, even if you decide to treat the atrial fibrillation. Finally, a rule of thumb I have used is that if the rate is less than 150, hypotension is unlikely to be the result of atrial fibrillation, whereas if the rate is greater than 150, the arrhythmia is probably at least a component of the patient’s shock. If the atrial fibrillation is long stranding, it is also less likely to be the cause of the instability. 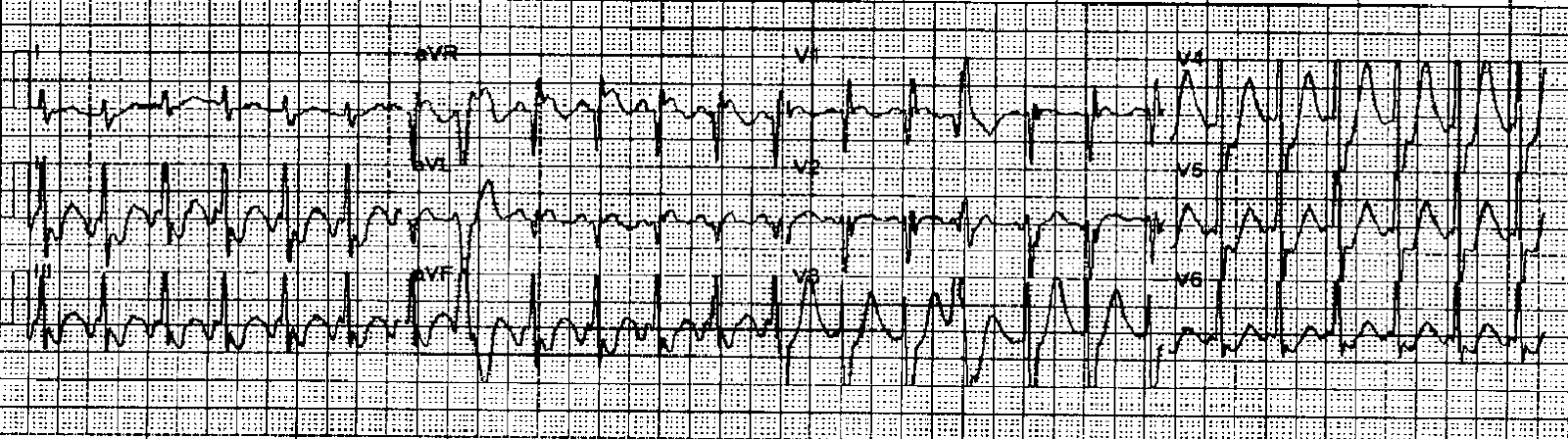
If there is an obvious alternate etiology for the hypotension (hemorrhage, sepsis, etc), I start by treating that. However, it can be very difficult to determine whether rapid atrial fibrillation is the cause of, or the result of hypotension. In these situations, the goal should be treating the underlying cause. In fact, the rapid heart rate is probably necessary to maintain an adequate cardiac output. If the patient’s hypotension and tachycardia are due to sepsis or hemorrhage, controlling the rapid heart rate is not going to help. What is your approach to unstable atrial fibrillation? My approach Is the atrial fibrillation the cause of the problem or just a symptom? His wife tells you this all started about 1 hour ago with complaints of dizziness and palpitations but no chest pain. The ECG is narrow complex and irregularly irregular. He is satting 100%, but is on a nonrebreather. The monitor reveals a heart rate of approximately 205, but it jumps around a lot from beat to beat. The chart in your hand says that he has a history of hypertension and hyperlipidemia, but is otherwise healthy. You walk into the room and see a grey, diaphoretic man, who you later find out is 67 years old. 
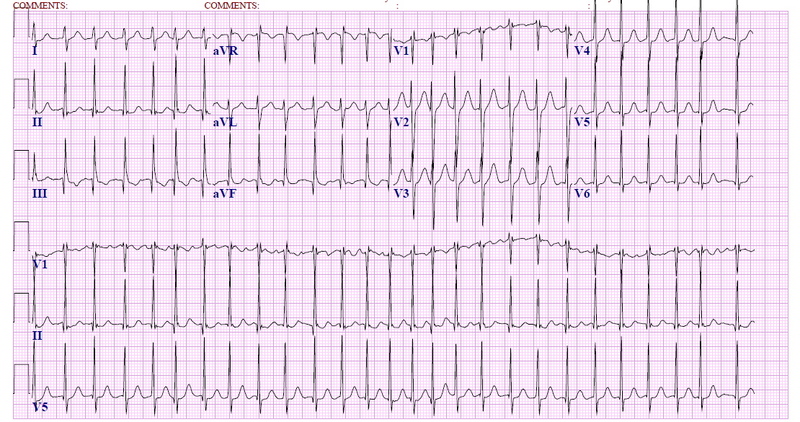
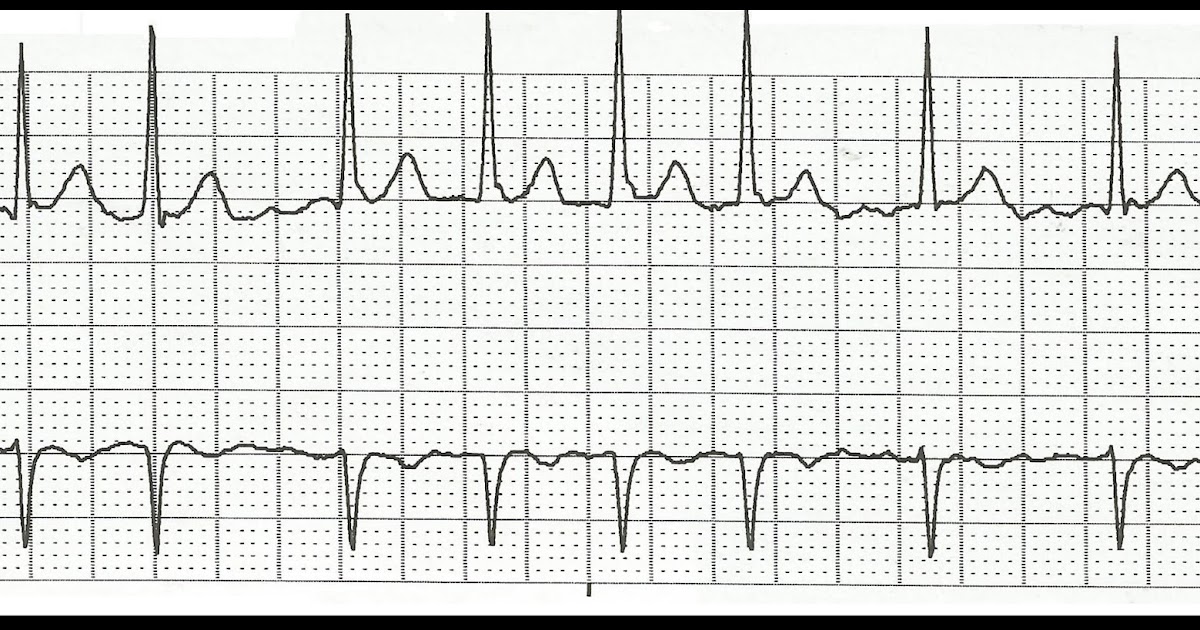
The charge nurse asks you to see one more patient, who she thinks has SVT, before you head home. Your relief is currently managing a sick appearing patient in status epilepticus. But over time, atrial flutter often returns since cardioversion alone does not correct the underlying causes of an abnormal heart rhythm.You are finishing up your charts and getting ready to head home for the night. This commonly will restore your normal heart rhythm.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
